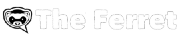People with both mental health and addiction issues are still facing a postcode lottery for treatment, despite national guidance that should guarantee everyone gets support to address Scotland’s drug death crisis, according to a new report.
The latest findings from the Mental Welfare Commission (MWC) for Scotland – a statutory body set-up to uphold the mental health act – come more than a year after the commission’s review of the provision of services for those simultaneously experiencing drug and mental health issues called for better universal support.
Campaigners have told The Ferret that people’s lives have been upended or put in danger when they could not access the care they needed for their mental health because they were using drugs.
The commission’s initial review, published in September 2022, found people both using drugs and suffering from mental illness were being “bounced between services” and often falling through the gaps, sometimes with tragic consequences.
Ninety per cent of the GPs who responded to the review said they had experienced difficulties in referring patients to both mental health services and addiction services, including when the person appeared to be in crisis.
Health authorities agreed to implement the review’s recommendations, which were also endorsed by Scottish Government national standards for people looking for treatment for their drug use.
But when the MWC for Scotland followed up with health authorities a year later as part of its “closure report” to assess progress made, it found many had still to fully implement changes, which it is claimed could save lives.
The report recorded a mixed picture. Some health and social care partnerships and health boards said they had already put in place measures to ensure that people with both mental health and drug issues get treatment, in line with the recommendations.
Not enough is changing and there is still not enough joined-up thinking.
Sandra Holmes, Families Campaign for Change
Some health and social care partnerships had moved both drug and mental health services into one building and one had invited members of the alcohol and drug recovery team to attend community mental health team meetings to help them work together.
But despite Scotland’s ongoing public health emergency in relation to drug deaths, about a quarter of health services had not yet implemented plans. One said they did not expect to start work on this until November this year and another said the services already worked well together and were unsure that a protocol was needed.
Dr Arun Chopra, medical director of MWC for Scotland, said the recommendation for all health authorities to develop written agreements to treat people with both mental health and drug use issues was based on evidence from the National Confidential Inquiry into Suicide and Safety in Mental Health. It found these protocols reduced deaths.
“We found the various health authorities are all in very different places,” he said. “Some have done a lot of work. Others are aiming to implement protocols in March 2024. But others are further off – one said it would be November 2024.
“It was positive that no one said they wouldn’t do it. But given the work on this is so important we were very surprised to see such a range of responses. We are still in the midst of a public health emergency so there is an urgency here.”
The commission will continue to raise the issue with health boards, he added, as well as staying in touch with its advisory group – who have experience of the issue – as part of its monitoring process.
The Ferret has previously reported that people have been denied access to mental health care due to their drug use, including mothers who have had children taken into care because they have been unable to access appropriate help, sometimes for several years.
Sandra Holmes, of the grassroots group Families Campaign for Change – which supports the parents and loved ones of those struggling with their drug use – claimed that she was yet to see change on the ground.
“They are still just ticking the boxes,” she said. “But we see people being turned away from services all the time because they struggle with both mental health and addiction. The two things go hand in hand. I’m not sure I know of anyone who we help that doesn’t also have issues with their mental health.”
Recent cases dealt with by Holmes include supporting the family of one man who was admitted to hospital following a drug overdose. He said his flat had been taken over by drug dealers, he had built up serious drug debts and the impact had led to a mental health crisis. She stepped in and ensured he had a follow-up appointment with drug treatment services.
In another case the child of someone she was supporting jumped out of the window while in psychosis and ended up in hospital for four months after being told he was not ready for rehab due to his mental health issues.
“Not enough is changing and there is still not enough joined-up thinking,” Holmes added. “We need accountability and we need a 24/7 helpline for our loved ones, as well as for their families.”
A spokesperson for the Scottish Government said: “We welcome the Mental Welfare Commission Report and are committed to improving care for people with co-occurring mental health and substance use issues.
“We are funding Healthcare Improvement Scotland to ensure that every part of Scotland has joint working protocols in place to make sure that people don’t fall through the gaps of mental health and substance use support.”
Main image: KatarzynaBialasiewicz/iStock